The herpes simplex virus (HSV) can cause blisters and sores almost anywhere on the skin. These sores usually occur either around the mouth and nose, or on the genitals and buttocks.
OVERVIEW
HSV infections can be very annoying because they can periodically reappear. The sores may be painful and unsightly. For chronically ill people and newborn babies, the viral infection can be serious, but rarely fatal. There are two types of HSV – Type 1 and Type 2.
The Type 1 virus causes cold sores. Most people get Type 1 infections during infancy or childhood. They usually catch it from close contact with family members or friends who carry the virus. It can be transmitted by kissing, sharing eating utensils, or by sharing towels. The sores most commonly affect the lips, mouth, nose, chin or cheeks and occur shortly after exposure. Patients may barely notice any symptoms or need medical attention for relief of pain.
The Type 2 virus causes genital sores. Most people get Type 2 infections following sexual contact with an infected person. The virus affects anywhere between 5 and 20 million people, or up to 20 percent of all sexually active adults in the United States.
With either type of herpes simplex, you can spread lesions by touching an unaffected part of the body after toughing a herpes lesion.
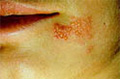
What is Herpes?
Herpes is the scientific name used for eight related A viruses of humans. Herpes simplex is related to the viruses that cause infectious mononucleosis (Epstein-Barr Virus), chicken pox and shingles (varicella zoster virus).
Herpes Simplex Virus Type 1
Often referred to as fever blisters or cold sores, HSV Type 1 infections are tiny, clear, fluid-filled blisters that most often occur on the face. Less frequently, Type 1 infections occur in the genital area. Type 1 may also develop in wounds on the skin. Nurses, physician, dentists, and other health care workers rarely get a herpetic sore after HSV enters a break in the skin of their fingers.
There are two kinds of infections – primary and recurrent. Although most people when exposed to the virus get infected, only 10% will actually develop sores or cold blisters when this infection occurs. The sores of a primary infection appear two to twenty days after contact with an infected person and can last from seven to ten days.
The number of blisters varies from one to a group of blisters. Before the blisters appear, the skin may itch or become very sensitive. The blisters can break as a result of minor injury, allowing the fluid inside the blisters to ooze and crust. Eventually, crusts fall off, leaving slightly red healing skin.
The sores from the primary infection heal completely and rarely leave a scar. However, the virus that caused the infection remains in the body. It moves to nerve cells where it remains in a resting state.
Many people will not have a recurrence. Others will have a recurrence either in the same location as the first infection or in a nearby site. The infections may recur every few weeks or less frequently.
Recurrent infections tend to be milder than primary infections. They can be set off by a variety of factors including fever, sun exposure, and a menstrual period. However, for many, the recurrence is unpredictable and has no recognizable cause.
Herpes Simplex Virus Type 2
Infection with herpes simplex virus Type 2 usually results in sores on the buttocks, penis, vagina or cervix, two to twenty days after contact with an infected person. Sexual intercourse is the most frequent means of getting the infection. Both primary and repeat attacks can cause problems including; a minor rash or itching, painful sores, fever, aching muscles and a burning sensation during urination. HSV Type 2 may also occur in locations other than the genital area, but is usually found below the waist.
As with Type 1, sites and frequency of repeated bouts vary. The initial episode can be so mild that a person does not realize that he or she has an infection. Years later, when there is a recurrence of HSV, it may be mistaken for an initial attack, leading to unfair accusations about the source of infection.
After the initial attack, the virus moves to nerve cells remaining there until set off again by a menstrual period, fever, physical contact, stress, or something else.
Pain or unusual tenderness of the skin may begin between one to several days before both primary and recurrent infections develop. This is called a prodrome.
How Are the HSV Infections Diagnosed?
The appearance of HSV is often so typical that no further testing is necessary to confirm an HSV infection. However, if the diagnosis is uncertain, as it may be in the genital or cervical areas, a swab from the infected skin (culture) may be taken and sent to the laboratory for analysis. Other laboratory tests available for diagnosis include specially treated scrapings that are examined under the microscope, and blood tests for antibodies. Some tests are only valid in the early stages, and more than one of these tests may be required to confirm the presence of herpes. Genital herpes can be mistaken for other diseases, including syphilis. A small number of women with genital herpes don’t know they have it because it occurs on the cervix which is not sensitive to pain.
How are Herpes Infections Treated?
There is no vaccine that prevents this disease from occurring. Oral anti-viral medications such as acyclovir, famciclovir, or valacyclovir have been developed to effectively treat herpes infections. These medications can be used to treat an outbreak or can be used for suppressing herpes recurrences. Lower doses may be helpful in reducing the number of herpes attacks in people with frequent outbreaks.
How Do You Prevent Transmission?
Between 200,000 and 500,000 people “catch” genital herpes each year and the number of Type 1 infections is many times higher. Prevention of this disease, which is contagious before and during outbreak, is important.
If tingling, burning, itching, or tenderness (signs of a recurrence) occur in an area of the body where you had a herpes infection, then that area should not contact other people. With mouth herpes, one should avoid kissing and sharing cups or lip balms. For persons with genital herpes, this means avoiding sexual relations, including oral/genital contact during the period of symptoms or active lesions. Condoms can help prevent transmission of genital herpes to your sexual partner.
Can Herpes be Spread if there is No Visible Sore?
Not only can herpes be spread if there is no sore, MOST herpes is transmitted in the absence of lesions! It is now estimated that over 80% of all genital herpes is transmitted when there isn’t anything on the skin and no symptoms. Patients have been aware for many years that if they kissed someone while having a fever blister or had sex with their partner while having an outbreak of genital herpes that they were likely to transmit the virus. Despite this knowledge, however, a 30% increase in the prevalence of HSV 2 infections was documented in the 1980s and 1990s. This increase is most likely due to the presence of HSV on the genital skin in the absence of lesions or symptoms. This phenomenon is known as “asymptomatic viral shedding” and has been demonstrated in well-controlled clinical investigations. Most recently, persons who never recall having had an outbreak of genital herpes, but who have had positive blood tests for antibodies to herpes, also have been demonstrated to “shed” the virus occasionally from lips or genital skin. It has been demonstrated that persons who take acyclovir daily have reduced amounts of the virus in the absence of symptoms or lesions. The same is probably true of the newer drugs, famciclovir and valacyclovir. It is logical that taking one of these three drugs everyday would reduce the chances of passing the virus to an uninfected partner, but this has not yet been proven.
Other Serious Implications of HSV
- Eye Infections – HSV may infect the eye and lead to a condition called herpes keratitis. There is pain and light sensitivity, a discharge, and a gritty sensation in the eye. Without prompt treatment, scarring of the eye may result. Fortunately, there are drugs available that are quite effective in eliminating infection and preventing severe scarring in the cornea. Any patient with a suspected eye infection from herpes should be seen immediately by an ophthalmologist.
- Infections in Pregnancy – A pregnant woman who has genital herpes at the time of childbirth may transmit the virus to her baby as it passes through the birth canal. If the birth occurs during the mother’s first episode of genital herpes, the baby may suffer severe damage. Women who know that they have had genital herpes or think they might have it during their pregnancy should tell their physicians so the baby can be protected.
Pregnant women should avoid sexual contact with a partner who has active genital herpes, (especially late in the pregnancy). The use of condoms is recommended for those who do not abstain.
The newborn can also be infected by exposure to the virus from non-genital lesions. If the mother or a person working in the nursery has active blisters on the lips or hands, the baby can become infected. Family members and friends with the active HSV should not handle the newborn child.
No special precautions need to be taken by the woman who has inactive herpes (genital or non-genital) at the time of delivery. Since the mother’s infection is not active, the infant is not at risk.
- HSV And The Seriously Ill – HSV can be life-threatening to the person who has cancer, a person who has had an organ transplant or anyone who has some other major illness, because their immunity to infections has been reduced.
Can Herpes be Cured?
While there are no known cures for herpes, clinical studies are now ongoing to attempt to reduce or possibly eliminate outbreaks. These experimental therapies, however, have no potential to eliminate the virus from the affected nerve. Therefore, these investigations are also attempting to determine if the rate of “asymptomatic viral shedding” can also be reduced.
